Terapia laserowa podprogowa to leczenie plamki
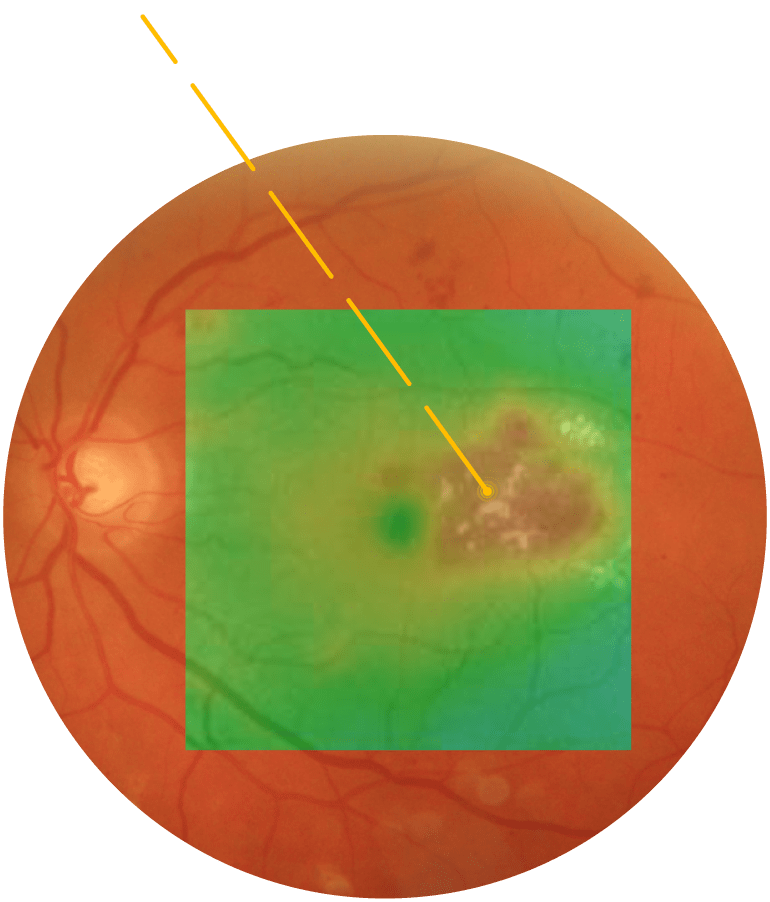
Leczenie plamki żółtej
Terapia laserowa SubLiminal jest obecnie techniką najczęściej stosowaną w przypadkach chorób naczyń krwionośnych siatkówki i chorób przebiegających z obrzękiem plamki żółtej, takich jak cukrzycowy obrzęk plamki żółtej (DME) i centralna surowicza chorioretinopatia (CSR).
Może też mieć zastosowanie w innych patologiach plamki żółtej, takich jak obrzęk plamki żółtej w przebiegu zakrzepu gałązki żyły środkowej siatkówki (BRVO) i polipoidalnej waskulopatii naczyniówkowej (PCV).
Wytyczne dotyczące leczenia
Leczenie laserowe techniką SubLiminal jest metodą dostarczania energii laserowej do siatkówki i uzyskania biostymulacji przy minimalnym trwałym uszkodzeniu cieplnym tkanki siatkówki. Metoda ta polega na dostarczeniu szeregu impulsów w odstępie czasu wystarczającym do rozproszenia ciepła tak, aby zapobiec trwałemu uszkodzeniu siatkówki. W odróżnieniu od konwencjonalnej terapii laserowej plamki żółtej nie powstaje bliznowacenie, które można byłoby wykryć w badaniu klinicznym OCT lub angiogramie.
Poniżej znajdują się wytyczne dotyczące laseroterapii SubLiminal, przygotowane przez dr. Victora Chonga (UK).

Retina Treatment: Subliminal Treatment Procedure

Basic Principles of MicroPulse Lasers

Dane kliniczne
Centralna chorioretinopatia surowicza (CSC)
Centralna chorioretinopatia surowicza (CSC) jest jedną z najczęstszych przyczyn utraty wzroku na tle zaburzenia siatkówki. Cechuje się surowiczym odwarstwieniem siatkówki neurosensorycznej wtórnym do co najmniej jednej zmiany ogniskowej nabłonka barwnikowego siatkówki (RPE)1. Jest to jedna z najczęstszych, zagrażających widzeniu retinopatii obok AMD, retinopatii cukrzycowej i zakrzepu gałązki żyły środkowej siatkówki2.
W ostrej CSC odwarstwienie jest spowodowane wyciekiem ogniskowym poprzez RPE. Zazwyczaj zaburzenie ustępuje samoistnie w ciągu kilku tygodni3. Jednakże przewlekła CSC może prowadzić do trwałego uszkodzenia struktur i znaczącej utraty widzenia centralnego456.
Dostępne są różne możliwości leczenia, lecz nie ma „złotego standardu” w przypadku przewlekłej CSC7:
- Konwencjonalna fotokoagulacja ma zastosowanie w wyciekach poza dołkiem, lecz wiąże się ze znaczącymi uszkodzeniami i może prowadzić do objawowych mroczków oraz neowaskularyzacji naczyniówkowej.
- Można również zastosować laseroterapię PDT, jednak nawet przy ustawieniu niskich wartości, wiąże się ona z licznymi działaniami niepożądanymi, takimi jak atrofia RPE, neowaskularyzacja naczyniówkowa, niedokrwienie warstwy naczyń włosowatych naczyniówki oraz przejściowe zaburzenie czynności plamki żółtej.
- Terapia żółtym światłem laserowym SubLiminal® o długości 577 nm wydaje się obiecującą strategią leczenia8.
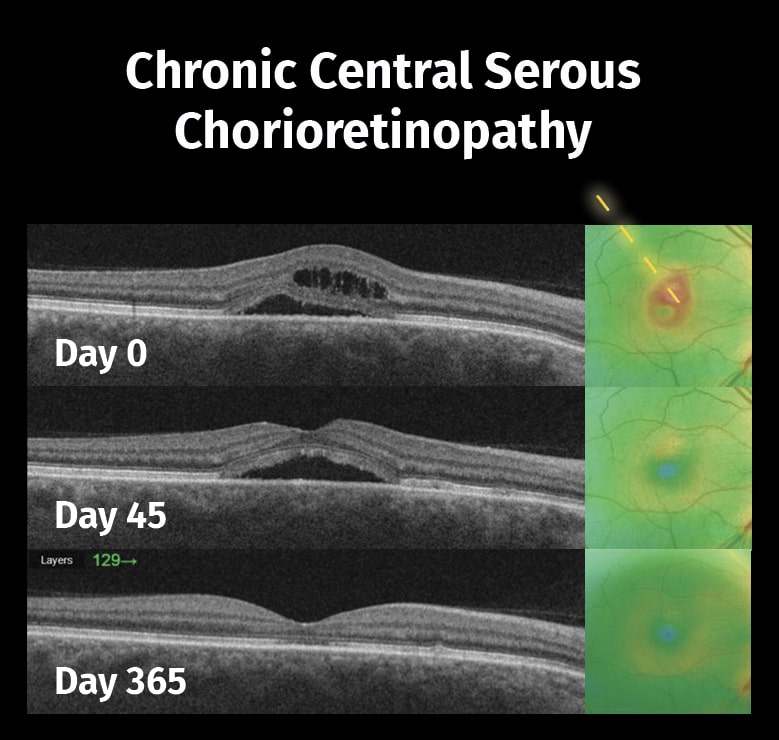
Ryciny dzięki uprzejmości dr. n. med. Alejandra Filloy Rius – Tarragona, Hiszpania

Lasers for Retina

Subthreshold laser therapy guidelines for retinal diseases

Central Serous Chorioretinopathy: Can it be treated without Visudyne?
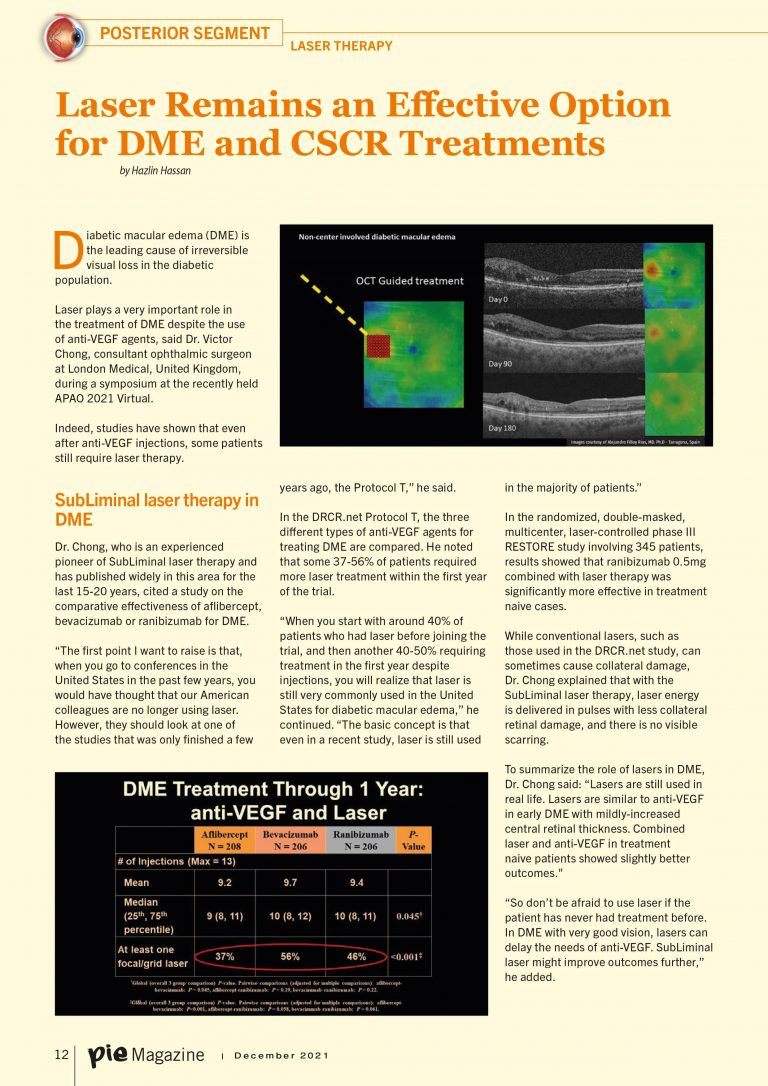
Laser Remains an Effective Option for DME and CSCR Treatments

SubLiminal Laser Therapy for CSC

Safe and Effective Laser Therapies: Targeting Retinal Diseases Amidst COVID-19

The Role of the New Generation of Lasers in Retina

Efficacy and safety of subthreshold micropulse laser compared with threshold conventional laser in CSC

Lessons Learned: SubLiminal Laser Therapy for Chronic CSC

What is the role of Easyret subthreshold laser in macular diseases?

SubLiminal laser for DME and CSC: when and how?

SubLiminal laser for cCSC management

Yellow subthreshold laser vs pdt in eyes with CCSC

Subliminal laser for the treatment of Central Serous Chorioretinopathy

Our first year of lessons learnt with SubLiminal laser for CCSC and DME

The Role of Subthreshold Laser Therapy in the Age of Intravitreal Injections

Subthreshold Laser Therapy: An Overview of Treatment Guidelines & Experience with the Easyret Laser
Cukrzycowy obrzęk plamki (DME)
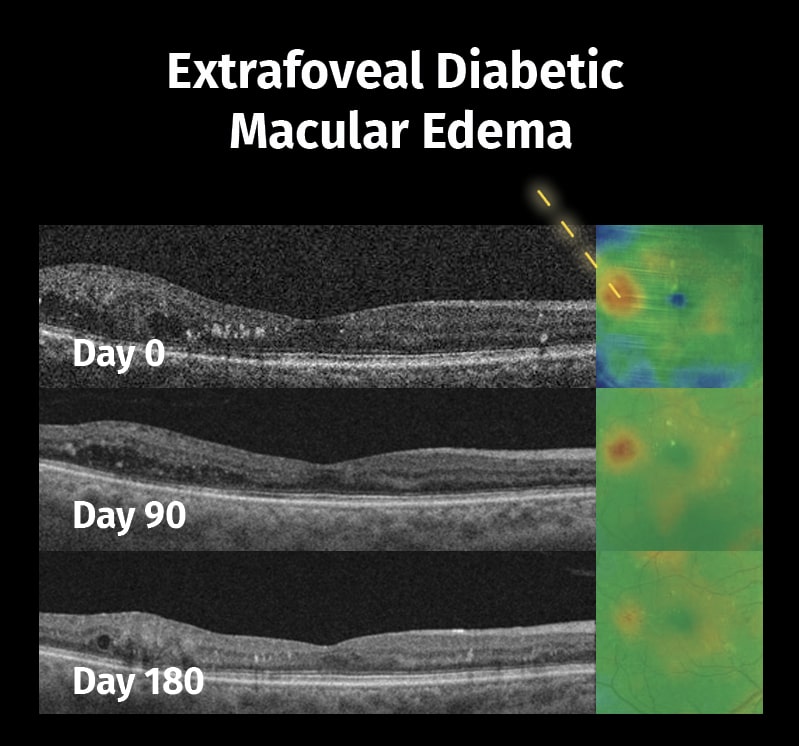

Managing DME With Subthreshold Laser

Lasers for Retina

Laser Remains an Effective Option for DME and CSCR Treatments

SubLiminal Laser for Center-Involving Diabetic Macular Edema

An Exciting Journey in SubLiminal Laser Treatment Therapy for DME

Subthreshold yellow laser for fovea-involving diabetic macular edema in a series of patients with good vision

Macular laser photocoagulation in the management of diabetic macular edema: Still relevant in 2020?

Management of cystoid macular edema secondary to retinitis pigmentosa via subliminal micropulse yellow laser

Comparison of ranibizumab and subthreshold micropulse laser in treatment of macular edema secondary to branch retinal vein occlusion

What is the role of Easyret subthreshold laser in macular diseases?
Controversies on Modern Laser Treatments for Retina and Vitreous
SubLiminal Laser for predominantly non-center involving DME?

Transfoveal SubLiminal Laser treatment for CSC

SubLiminal laser for DME and CSC: when and how?

Fovea-Involving DME: Reasons for the subliminal approach

Our first year of lessons learnt with SubLiminal laser for CCSC and DME

The Role of Subthreshold Laser Therapy in the Age of Intravitreal Injections

Subthreshold Laser Therapy: An Overview of Treatment Guidelines & Experience with the Easyret Laser
Zwyrodnienie plamki żółtej związane z wiekiem
Zwyrodnienie plamki żółtej związane z wiekiem jest główną przyczyną nieodwracalnej utraty wzroku wśród osób starszych.
Sucha postać AMD występuje u 80-90% pacjentów z AMD.
We wczesnych stadiach AMD na siatkówce, poniżej plamki żółtej, tworzą się małe białe lub żółtawe złogi, nazywane druzami, z czasem prowadząc do jej zwyrodnienia.
Twarde druzy są małymi zmianami o wyraźnych granicach, które obserwuje się w populacji zdrowych seniorów.
Miękkie druzy są większe, a ich granice są mniej wyraźne (przypominają watę). Przeważnie mają charakter patologiczny i nie występują u młodych, zdrowych osób.
Nie powstała jeszcze skuteczna metoda leczenia druzów, istnieją jednak obserwacje kliniczne wskazujące na zanikanie druzów pod wpływem podprogowej laseroterapii, co pozwala zapobiec progresji patologii.
Trwają obecnie badania kliniczne dotyczące tego zagadnienia.

SubLiminal laser for AMD

Expanding clinical application of SubLiminal laser therapy
Idiopatyczna polipoidalna waskulopatia naczyniówkowa (IPCV)
Idiopatyczna polipoidalna waskulopatia naczyniówkowa (IPCV) jest chorobą naczyń krwionośnych naczyniówki.
Cechuje się występowaniem polipoidalnych zmian o charakterze tętniaka i rozgałęzionej sieci naczyń krwionośnych w naczyniówce. Może prowadzić do surowiczego lub krwotocznego odwarstwienia nabłonka barwnikowego siatkówki (PED), epizodów wysiękowego odwarstwienia siatkówki oraz podsiatkówkowego wysięku i krwawienia.
To zaburzenie jest uważane za wariant neowaskularnej AMD.
IPCV występuje względnie często u obu płci w populacji azjatyckiej i afroamerykańskiej.
Dowody skuteczności :
- U pacjentów z objawami IPCV można uzyskać całkowitą regresję bez poważnej utraty wzroku dzięki zastosowaniu terapii fotodynamicznej (PDT) i anty-VEGF.
- Terapia światłem laserowym SubLiminal o długości 577 nm może stanowić leczenie dodatkowe IPCV w przypadkach suboptymalnej odpowiedzi na środki anty-VEGF.

Efficacy of SubLiminal laser in IPCV Aflibercept resistant cases
Lekarze
Porozmawiaj o podprogowejterapii laserowej





Bibliografia
Central serous chorioretinopathy (CSCR) is a common retinal cause of vision loss. This review surveys the epidemiology, risk factors, clinical presentation, natural history and pathophysiology of CSCR. Studies suggest an annual incidence rate of 10 per 100 000 in men, with CSCR occurring six times more commonly in men compared with women. Most acute CSCR cases resolve spontaneously within 2–3 months. Prognosis is highly dependent on presenting visual acuity; patients with initial visual acuities of 6/6 remain at that level, while patients with initial visual acuities of less than 6/9 recover on average two to three Snellen lines over the next few years. The main risk factors for CSCR are systemic corticosteroid use, type A personality, pregnancy and endogenous Cushing’s syndrome. The pathophysiology of CSCR remains obscure, although disorders in both the choroidal circulation and retinal pigment epithelium are implicated.
Central serous chorioretinopathy (CSC) is a disease of the retina characterized by serous detachment of the neurosensory retina secondary to one or more focal lesions of the retinal pigment epithelium (RPE). CSC occurs most frequently in mid-life and more often in men than in women. Major symptoms are blurred vision, usually in one eye only and perceived typically by the patient as a dark spot in the centre of the visual field with associated micropsia and metamorphopsia. Normal vision often recurs spontaneously within a few months. The condition can be precipitated by psychosocial stress and hypercortisolism. Ophthalmoscopic signs of CSC range from mono- or paucifocal RPE lesions with prominent elevation of the neurosensory retina by clear fluid – typical of cases of recent onset – to shallow detachments overlying large patches of irregularly depigmented RPE.
Data are presented from 27 patients (34 eyes) with central serous choroidopathy who were followed up for an average of 23 months without therapeutic intervention. The detachment completely resolved in all cases. The average duration of detachment was three months. In all eyes, the visual acuity returned to 20/40 or better, and in all but two eyes, the final visual acuity was 20/30 or better. Central serous choroidopathy is essentially a benign and self-limited disorder, and treatment by photocoagulation is seldom needed.
The Wilmer Retinal Vascular Center’s experience with central serous chorioretinopathy from 1970 to the end of 1979 was reviewed and compared with previous studies. Retrospective analysis of 73 patients seen at follow-up suggests no clinically significant effect of focal argon laser photocoagulation on final visual acuity or recurrence rate. Patients with initial visual acuity of 20/20 remained at that level, and patients with initial visual acuity of less than 20/30 gained, on average, two to three Snellen lines at follow-up. Approximately one-third of both untreated and treated patients had recurrence or presumed persistence during the follow-up period. With the inclusion of episodes that occurred before the first Wilmer Institute visit about half of each group had recurrence or presumed persistence. Recurrences were most often due to leakage from a site within one disc diameter of the original site of leakage.
In a prospective randomised trial of argon laser photocoagulation in the management of central serous retinopathy, long-term follow-up (6.4 to 12.1 years) revealed no evidence that treatment significantly influenced the visual outcome as measured by the Snellen chart and by the Farnsworth-Munsell 100-hue test. Treatment did not reduce either the recurrence rate or the prevalence of chronic disease. Complications of treatment were uncommon. The justification for argon laser photocoagulation appears to be limited to the hastening of symptomatic relief by earlier resolution of serous detachment.
Background: To evaluate risk factors for the recurrence of serous macular detachment in untreated patients with central serous chorioretinopathy (CSC).
Methods: Retrospective review of untreated CSC patients with a follow-up of ≥3 years. Patient demographics, visual outcome and risk factors for the recurrence of CSC were analyzed.
Results: Seventy-three eyes of 73 patients were included, and the mean age was 44.6 years. At baseline, the mean logMAR best corrected visual acuity (BCVA) was 0.30. After a mean follow-up of 72 months, the mean final logMAR BCVA was 0.32. The difference between the final and baseline BCVAs was not statistically significant (p = 0.79). At the last follow-up, 9 (12.3%) eyes showed improved vision of ≥2 lines, and 12 (16.4%) showed a worsening of ≥2 lines. During follow-up, 38 (52.1%) patients experienced ≥1 episode of CSC recurrence. Multivariate Cox regression analysis showed that patients with a history of psychiatric illness (adjustment disorder and depression) were associated with an increased risk of CSC recurrence (hazard ratio = 3.5, p = 0.011).
Conclusions: The long-term visual prognosis of CSC is fair without treatment, and a significant proportion of patients developed recurrence of CSC. A history of psychiatric illness is associated with an increased risk of CSC recurrence.
Purpose: To assess treatment with a 577-nm subthreshold micropulse laser (SML) in patients with chronic central serous chorioretinopathy (cCSC).
Methods: This retrospective study included 38 patients treated with a 577-nm SML (Supra Scan; Quantel Medical) for cCSC. We included a subgroup of 18 patients with persistent subretinal fluid (SRF) after photodynamic therapy (PDT). Assessment included visual acuity (VA), central retinal thickness (CRT) and resolution of SRF.
Results: At the last follow-up (mean 5 months), 74% of patients responded to therapy. The CRT decreased after treatment (mean CRT -115 µm, p < 0.001) and VA improved (mean logMAR -0.06, p = 0.039). No laser burns were detected with any imaging modality. In the subgroup of patients resistant to PDT, 61% of patients responded to therapy with a decrease in CRT (mean CRT -75 µm, p = 0.019).
Conclusions: The 577-nm SML is an effective treatment for cCSC even in patients without sufficient improvement after PDT.
Purpose: To compare the short-term treatment outcome of the 577 nm subthreshold micropulse laser (SML) and half-dose photodynamic therapy (PDT) in patients with chronic central serous chorioretinopathy (cCSC) and persistent subretinal fluid (SRF).
Methods: This retrospective study included 100 eyes of 100 consecutive patients who were treated with the 577 nm SML (Supra Scan, Quantel Medical) (n=42) or half-dose PDT (n=58) for cCSC. The treatment was applied at the leakage sites in the fluorescein and indocyanine green angiography. The treatment success was evaluated 6 weeks after treatment using best-corrected visual acuity, central retinal thickness, and resolution of SRF in spectral domain optical coherence tomography.
Results: Patients showed treatment response more often in the SML group compared with the PDT group (treatment response after SML: 33 eyes (79%), PDT: 34 eyes (59%), P=0.036, χ2 test). The CRT decreased significantly after both treatments (mean CRT before SML: 445±153 μm, after SML: 297±95, Po0.001; mean CRT before PDT: 398±88 μm, after PDT: 322±93 μm, Po0.001, Wilcoxon’s signed-rank test). The decrease in CRT was statistically significantly higher in the SML group (decrease in CRT after SML: − 148±163 μm, after PDT: −76±104 μm, P=0.041, Mann–Whitney U-test).
Conclusions: Both the half-dose PDT and the 577 nm SML are potent treatments for cCSC with persistent SRF. More patients showed treatment response to the SML treatment and SML leads to a greater decrease in CRT.
Objective: To examine the global prevalence and major risk factors for diabetic retinopathy (DR) and vision-threatening diabetic retinopathy (VTDR) among people with diabetes.
Research design and methods: A pooled analysis using individual participant data from population-based studies around the world was performed. A systematic literature review was conducted to identify all population-based studies in general populations or individuals with diabetes who had ascertained DR from retinal photographs. Studies provided data for DR end points, including any DR, proliferative DR, diabetic macular edema, and VTDR, and also major systemic risk factors. Pooled prevalence estimates were directly age-standardized to the 2010 World Diabetes Population aged 20-79 years.
Results: A total of 35 studies (1980-2008) provided data from 22,896 individuals with diabetes. The overall prevalence was 34.6% (95% CI 34.5-34.8) for any DR, 6.96% (6.87-7.04) for proliferative DR, 6.81% (6.74-6.89) for diabetic macular edema, and 10.2% (10.1-10.3) for VTDR. All DR prevalence end points increased with diabetes duration, hemoglobin A(1c), and blood pressure levels and were higher in people with type 1 compared with type 2 diabetes.
Conclusions: There are approximately 93 million people with DR, 17 million with proliferative DR, 21 million with diabetic macular edema, and 28 million with VTDR worldwide. Longer diabetes duration and poorer glycemic and blood pressure control are strongly associated with DR. These data highlight the substantial worldwide public health burden of DR and the importance of modifiable risk factors in its occurrence. This study is limited by data pooled from studies at different time points, with different methodologies and population characteristics.
Subthreshold, or tissue-sparing, laser therapy is a subject of interest to retinal specialists worldwide. Today, micropulse technology with 810 nm and 577 nm lasers is used to produce a therapeutic treatment without inducing intraretinal damage detectable on clinical examination during or after treatment. The controlled laser delivery of micropulse technology affords treatment options for diabetic macular edema(DME), proliferative diabetic retinopathy (PDR), central erous chorio retinopathy (CSR), macular edema secondary to branch retinal vein occlusion (BRVO), and even glaucoma. This review will explain micropulse technology and focus on its benefits and challenges in the treatment of retinal disorders.
Purpose: This pilot study aimed to evaluate the efficacy and safety of subthreshold micropulse yellow (577-nm) laser photocoagulation (SMYLP) in the treatment of diabetic macular edema (DME).
Methods: We reviewed 14 eyes of 12 patients with DME who underwent SMYLP with a 15% duty cycle at an energy level immediately below that of the test burn. The laser exposure time was 20 ms and the spot diameter was 100 µm. Laser pulses were administered in a confluent, repetitive manner with a 3 × 3 pattern mode.
Results: The mean follow-up time was 7.9 ± 1.6 months. The baseline-corrected visual acuity was 0.51 ± 0.42 logarithm of the minimum angle of resolution (logMAR), which was improved to 0.40 ± 0.35 logMAR (p = 0.025) at the final follow-up. The central macular thickness at baseline was 385.0 ± 111.0 µm; this value changed to 327.0 ± 87.7 µm (p = 0.055) at the final follow-up.
Conclusions: SMYLP showed short-term efficacy in the treatment of DME and did not result in retinal damage. However, prospective, comparative studies are needed to better evaluate the efficacy and safety of this treatment.
Keywords: Diabetic retinopathy; Laser therapy; Macular edema.